Written by Sophia Navarro
Spring 2018
 The undergraduate Public Health program at U.C. Berkeley stresses that one’s environment is central to their health. Since being introduced to this concept, I’ve been eager to understand the interaction between place, resource availability, and the policies that make up the surrounding environment with the health of different members of a community. The field of public health argues that some members of a population are disproportionately affected by certain health outcomes, not because of innate differences between groups of people, but rather because of the underlying social determinants of health. The social determinants of health are the physical, economic, and social conditions in the environment in which people live, work, and play that affect health, such as job opportunities, residential segregation, public safety, access to quality education, and public transportation. Groups with particular vulnerability to poor health outcomes include the economically disadvantaged, racial and ethnic minorities, pregnant women, children, the elderly, the immunocompromised, and those with chronic health conditions. Major goals in public health focus on closing the gaps in access to resources and reducing the unfair and avoidable health disparities between groups of people, which are defined as health inequities. Programs that work towards eliminating these differences ensure that every member of a community has the same potential to reach their optimal level of health.
The undergraduate Public Health program at U.C. Berkeley stresses that one’s environment is central to their health. Since being introduced to this concept, I’ve been eager to understand the interaction between place, resource availability, and the policies that make up the surrounding environment with the health of different members of a community. The field of public health argues that some members of a population are disproportionately affected by certain health outcomes, not because of innate differences between groups of people, but rather because of the underlying social determinants of health. The social determinants of health are the physical, economic, and social conditions in the environment in which people live, work, and play that affect health, such as job opportunities, residential segregation, public safety, access to quality education, and public transportation. Groups with particular vulnerability to poor health outcomes include the economically disadvantaged, racial and ethnic minorities, pregnant women, children, the elderly, the immunocompromised, and those with chronic health conditions. Major goals in public health focus on closing the gaps in access to resources and reducing the unfair and avoidable health disparities between groups of people, which are defined as health inequities. Programs that work towards eliminating these differences ensure that every member of a community has the same potential to reach their optimal level of health.
The influence of the food environment
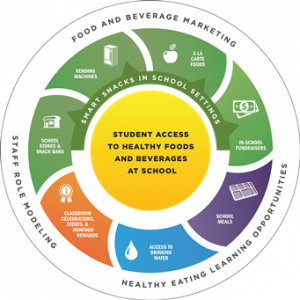 Working at the Nutrition Policy Institute (NPI) has given me the opportunity to explore the significance of the nutrition environment, which fuses my interests for public health and food systems via nutrition. We all know that food can influence our health: consuming healthy foods can make us healthy and consuming unhealthy foods can make us unhealthy. However, not everyone has the ability to access to the same types of healthy food choices, which is where we begin to see health disparities. Oftentimes, when we blame individuals for eating poorly, we ignore the fact that their environment may not support healthy options. This is why we must begin to look upstream for the causes of health disparities rather than trying to correct for poor health behaviors. Thus, understanding the nutrition environment becomes key to reducing health disparities related to dietary illnesses such as obesity, diabetes, and cardiovascular disease. The food environment includes the places and settings where people can consume food at the market, community, and consumer level. While past research has focused heavily on the individual consumption level, today more studies are investigating the roles of policies and programs on nutrition.
Working at the Nutrition Policy Institute (NPI) has given me the opportunity to explore the significance of the nutrition environment, which fuses my interests for public health and food systems via nutrition. We all know that food can influence our health: consuming healthy foods can make us healthy and consuming unhealthy foods can make us unhealthy. However, not everyone has the ability to access to the same types of healthy food choices, which is where we begin to see health disparities. Oftentimes, when we blame individuals for eating poorly, we ignore the fact that their environment may not support healthy options. This is why we must begin to look upstream for the causes of health disparities rather than trying to correct for poor health behaviors. Thus, understanding the nutrition environment becomes key to reducing health disparities related to dietary illnesses such as obesity, diabetes, and cardiovascular disease. The food environment includes the places and settings where people can consume food at the market, community, and consumer level. While past research has focused heavily on the individual consumption level, today more studies are investigating the roles of policies and programs on nutrition.
My work at NPI
NPI is a part of the University of California’s division of Agriculture and Natural Resources. At NPI, we “conduct research that informs nutrition policy and programs for healthy children, families and communities” and envision “a world where healthy food, beverages and opportunities for physical activity are convenient, accessible, affordable and sustainable.” While interning at NPI, I worked on several ongoing projects, including a study called Healthy Beverages in Childcare: Putting Policy into Practice and a study of School Foodservice Redesign to Improve Meal Participation & Dietary Intake.
Healthy Beverages in Childcare: Putting Policy into Practice Study
The Healthy Beverages in Childcare study is based on the fact that nearly 1 in 4 American children between the ages of 2 to 5 begin elementary school overweight or obese and that the introduction of healthy foods, beverages, and practices early on in life can lead to long-lasting healthy behaviors. Over 70% of these children spend their time in childcare centers and homes outside of their own home and because these childcare settings provide daily nutrition for the children under their care, they are the ideal environment to implement program and policy interventions to target obesity prevention. As of 2012, California has adopted a policy called Healthy Beverages in Childcare Act which regulates the amount and type of beverages that may be served to children in California childcare facilities. The law promotes drinking water and prohibits sugar sweetened beverages, juice, and 2% and full-fat milk for children aged 2 years and older. However, one challenge is that not many childcare employees are in compliance with this policy. In response to this, NPI initiated the development and evaluation of an online training on healthy beverages in California childcare centers across Alameda, Contra Costa, Santa Cruz, San Mateo, San Francisco, Merced, Stanislaus, Tulare, Kings, Santa Barbara, and San Luis Obispo Counties. I have contributed to this project through participant outreach and recruitment and by evaluating surveys which will be used to assess the online trainings. I also had the opportunity to search for existing surveys used to asses food purchasing behaviors and transform my results into a literature review, which allowed me to familiarize myself with a variety of nutrition policies, programs, study interventions, and surveys and led me to collaborate with researchers from universities and institutions across the world.
Study of School Foodservice Redesign to Improve Meal Participation & Dietary Intake
 I also had the opportunity to conduct research in a study assessing the impact new school foodservice redesigns in 24 middle and high schools in San Francisco Unified School District (SFUSD) on school lunch participation, the quality of student diet as reflected by fruit and vegetable consumption, return on investment, and sustainability of the intervention. The interventions included a combination of SmartMeal technology platforms, distributed points of sale, and staff promotion of school meals. A team of NPI staff, undergraduate volunteers, SFUSD Student Nutrition Service employees, and I recorded information on how many students participated in school lunch, which foods were chosen by students at which point of sale, and which foods were actually consumed by analyzing residual plate waste. In general, most students who participate in school lunch programs have a specified low-income status or come from families who do not have the time to prepare homemade meals for their children due to multiple obligations like working multiple jobs. Returning to a public health perspective, these children have a higher risk for adverse dietary-related health impacts like obesity compared to their more economically advantaged peers whose parents can provide them healthy, homemade meals on a daily basis. For these reasons, NPI’s research into effective ways to encourage healthy eating in the school environment is extremely impactful for health outcomes later on in a child’s life.
I also had the opportunity to conduct research in a study assessing the impact new school foodservice redesigns in 24 middle and high schools in San Francisco Unified School District (SFUSD) on school lunch participation, the quality of student diet as reflected by fruit and vegetable consumption, return on investment, and sustainability of the intervention. The interventions included a combination of SmartMeal technology platforms, distributed points of sale, and staff promotion of school meals. A team of NPI staff, undergraduate volunteers, SFUSD Student Nutrition Service employees, and I recorded information on how many students participated in school lunch, which foods were chosen by students at which point of sale, and which foods were actually consumed by analyzing residual plate waste. In general, most students who participate in school lunch programs have a specified low-income status or come from families who do not have the time to prepare homemade meals for their children due to multiple obligations like working multiple jobs. Returning to a public health perspective, these children have a higher risk for adverse dietary-related health impacts like obesity compared to their more economically advantaged peers whose parents can provide them healthy, homemade meals on a daily basis. For these reasons, NPI’s research into effective ways to encourage healthy eating in the school environment is extremely impactful for health outcomes later on in a child’s life.
Future Work
I have truly enjoyed working at NPI this semester and I am very excited to be able to continue working with them over the summer. Coming into NPI, I knew I had a passion for improving public health through nutrition, but my experience this semester has reaffirmed by drive for public health nutrition. In the following Fall 2018 semester, I will be taking a graduate-level course on Maternal and Child Nutrition to further my understanding of the nutrition environment and its critical impact on pregnant women and children throughout the lifecycle. In the next few years, I hope to attend graduate school to earn my Master’s in Public Health Nutrition and continue to reduce health inequities and dietary-related illnesses through better policies, programs, and interventions across communities, organizations, and institutions.


